AP
NOS News••Rate
-
Marty Giles
Online editor
-
Marty Giles
Online editor
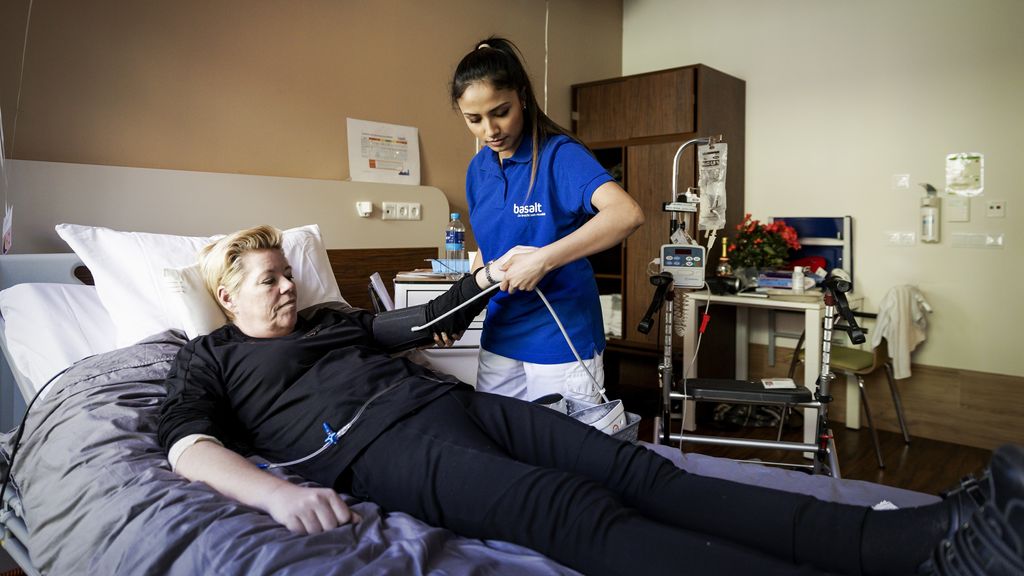
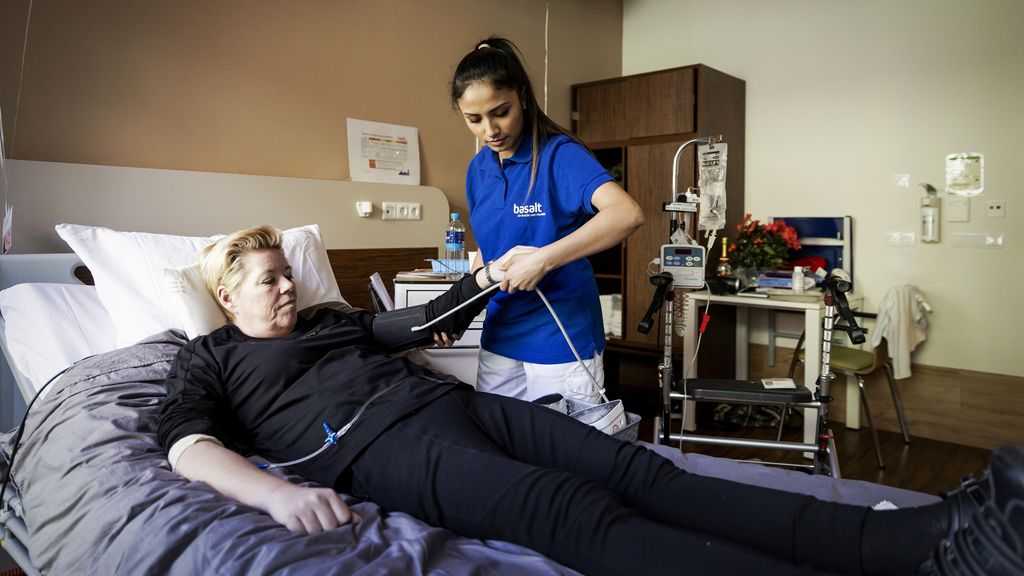
In March 2020, Tjitske Jaarsma* contracted the coronavirus through her husband. She developed a cough that turned into severe shortness of breath. At home, she is gasping for breath and eventually has to go to the hospital three times. Her daughter was also injured. More than two years later, the two still suffer from a host of complaints: fatigue, shortness of breath, and poor condition. “Just do something and you’ll be tired again.”
Jarsma and her daughter have now been diagnosed with COVID-19, or long-term complaints after infection with Corona. Little is known about lung covid, also known as post-covid syndrome. Experts talk about a range of complaints that can vary from person to person. Who has contracted pneumonia is unknown. We also don’t know how many people in the Netherlands walk around with residual complaints.
Pulmonologist Merel Hellemons (Erasmus MC) estimates that this could concern hundreds of thousands of people. She’s talking about “huge numbers.” There are no exact numbers. The national government does not follow through.
Hellemons bases its estimate on data from the UK, where the national statistics agency publishes figures on Covid-19 lung disease monthly. In December, the agency assumed 2.2 million people had symptoms of COVID-19. This represents 3.4 percent of the population. After converting them to the Dutch population, it will be 600,000 people, this month’s figure is also mentioned In a briefing to members of the House of Representatives.
Hellemons sees many patients with post-Covid syndrome in her work. “COVID-19 can cause a huge number of complaints, but there are a number of symptoms that we hear most often: fatigue, problems concentrating. But shortness of breath and, in short, everything related to the brain (stimulus processing and headaches) also occur.”
Very heavy kettle
“For the first few months I couldn’t even lift the kettle, it was so heavy,” says Jarsma. Now she has good days and bad days, which makes it hard to live a normal life. “We were an active family until March 2020. Now we have to think about everything. For example, can I go to a birthday or not? If I go, I can only stay for an hour.” The supermarket just picks them up, and the housework is very hard. “The bathroom doesn’t look good and the windows haven’t been cleaned for a long time.”
Jarsma spends a lot of time at home with her daughter. Not everyone around her knows about their situation. “When I’m on the street, you don’t see me. What people don’t know is that afterward you’re lying on the couch, exhausted.”
“You live in a parallel world, as if you were separate from people who did not have COVID-19,” says Vivienne Matthies-Boon. She contracted the virus at the end of January, was admitted twice, and then recovered. But she suffered a setback in September. “In the summer I could walk outside for 20 minutes at a time, which was the limit. But at least I could do something. I’ve been bedridden since September.”
She continues, “I get up in the morning, I try to take a shower and then I have to go to bed again.” Matisse Boone is academic, but she rarely visits her place of work, Radboud University. She works a few hours a week from home, mostly from bed. “Physically I can’t handle it anymore. While I really would like to work. I have my dream job and have been working towards it for years.”
unknown
Jarsma and Matthijs-Bonn are frustrated that so little is known about the lung virus and that so little research is being done in the Netherlands. For starters, it’s unclear why they contract it, while others emerge unscathed from the infection. Science does not (yet) have an answer to this.
“There are a number of risk factors, such as being a woman, obesity, certain chronic diseases, and the severity of acute infections,” says Judith van Roosmalen, a professor of psychosomatics. “But the studies still contradict each other and this of course is still very general.” Smoking and living a busy life also seem to be risk factors.
Van Roosmalen (UMC Groningen) led a large study on COVID-19 lung disease earlier this year. It showed that one in eight patients still had complaints three to five months after infection.
Hellemons pulmonologist sees these patients in action. Remarkably, lung function is almost always normal. “There didn’t seem to be anything wrong with the lungs themselves.”
Regular checkups often find something abnormal. But that’s not the end of it, Hellemons says. “The stigma many patients face is that it’s all in their heads.”
More specific tests detect deviations. “We know from studies, for example, that the immune system is in overdrive. We also find abnormalities in the bacterial flora in the gut and an increased tendency to clot. Some patients notice that their heart rate increases by 40 beats when they stand up, a sign of disruption of regulatory processes. complex in the body. She continued, “Everything was found to be abnormal, but the common denominator, that’s hard to say.”
I speak to 28-year-olds who have moved back into the home because they need care.
Hellemons requests more Dutch research on the lung virus. She also believes there needs to be a greater understanding of what she calls the “silent epidemic”. “I talk to 28-year-olds who have come back to live at home because they need care. These people are very sick and misunderstood as well.”
forgotten group
The pulmonologist talks about a “forgotten group” that doesn’t get much attention now that society has opened up again. Matisse Boone realizes that: “When you hear that other people have gone to the pub or are going on holiday, you really think: ‘When will I ever be able to do something again'”. It makes you desperate, for example I don’t “I don’t know if I can make dinner birthday. The table can fit.”
Jarsma hopes her daughter will recover, and now she has to miss school more often. “Her life is on hold.”
Matthijs Bonn is mainly hoping for a better year. “Last week I tried to bike outside for ten minutes, and then I collapsed. You don’t feel like a human anymore. Being human means being outside, doing something with other people. But now it doesn’t work.”
*Tjitske Jaarsma’s name has been changed for privacy reasons.

“Lifelong zombie fanatic. Hardcore web practitioner. Thinker. Music expert. Unapologetic pop culture scholar.”